I call this era of my life The Fainting Season, when my body could not bear the gravity of the situation. When every sidestep, every bent gesture, ended in a heap. When sitting up was a head wound, a miscalculated ejection fraction, a failure to blush. My whole city is a marble roll down to the lake and I faint daily walking the slight incline to my house, my body wrestling me to the ground like a service dog. I faint in COVID screening line-ups and clinic parking lots, in the heat of every shower and the head rush of putting on shoes, in elevators and swimming pool changing rooms and airport wheelchair line-ups, mixing pancakes in my girlfriend’s kitchen and in heated arguments. Rare was the hospital visit I didn’t collapse somewhere in the transfer of my body from ambulance to ambulatory care.
Science says fainting is a protective measure when there is not enough blood to the brain to function. But historically, there’s been less curiosity about the mechanisms of blood loss beyond blunt trauma: maybe arrhythmia or dehydration, shock or social influence, puberty or pregnancy, a weak mind unable to wrangle a weak body. In Lancashire, in 1965, mass fainting in a girls’ school following a polio outbreak was attributed to “over-breathing”. In Columbia, in 2014, it was either post-vaccination complications from Gardasil or mass hysteria, depending who you ask. Virginia Woolf famously wrote On Being Ill after she fainted at a party, setting off what was, at the time, considered a bout of “nerves”.
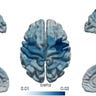
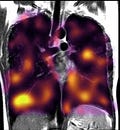
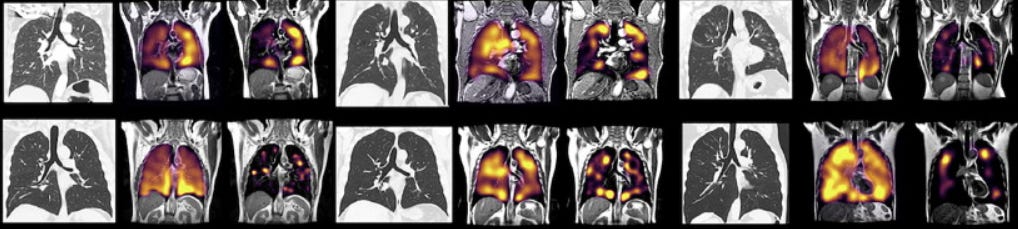
Today, research paints a different diagnostic picture with spectroscopy, MEG scans, and xenon gas MRIs. A University of Waterloo study found reduced oxygen saturation in the prefrontal cortex during cognitive tasks in people with prior symptomatic COVID. At Western University, researchers found impaired transit of oxygen from the tiny alveolar sacs of the lungs to red blood cells. As early as April 2020, studies found that COVID-19 both directly infects and ruptures the endothelium cells lining blood vessels and indirectly triggers inflammation. Without oxygen, and oxygenated blood, every function of the body breaks down, from mitochondrial energy production to the brain, which consumes an average of 49ml of oxygen per minute or 20 percent of the body’s total.
Fainting, or the near black-out of pre-syncope, is also common in Dysautonomia, an often post-viral disorder of the autonomic nervous system (ANS), which regulates involuntary but vital processes like heart rate, blood circulation, and body temperature. Dysautonomia (also known as POTS, one of the more common types) is present in up to 70% of Long COVID patients and notoriously difficult to get diagnosed and treated, with doctors preferring non-medical patient-managed interventions like compression tights and a high salt/high water diet. Dr. David Putrino (Mount Sinai Hospital, NYC) says the ANS is “a dial that your body uses to gently turn physiologically….from a state of rest to a state of activation and back”. When dysfunctional or damaged it becomes a heavy switch, abruptly triggering sympathetic activation and adrenaline surges or a parasympathetic state of disorientation, exhaustion, and indigestion, like Alice in Wonderland unable to settle at the appropriate size.
Some days I had both: flattened in bed but as stressed as if I were buried alive. My heart rate hit 170 bpm walking down the block; 140 making coffee. I’d wake up to a keening 120, shaking like a chihuahua. Before I got sick, my girlfriend teased me for trying hard at everything, but in tachycardia, although the heart tries harder, each beat is shorter, each pump of blood less effective.
In the 12th month of illness, I leave a medical appointment and stop at the grocery store next door. Disoriented, I forget the logic of shopping: how foods are clustered together or where to find carts. Conceiving of a whole meal and parsing it into purchasable pieces is impossible. Later, I will learn the bio-mechanical mechanisms behind this moment: how I’m losing blood to the brain the longer I stand still, staring at jars with labels I can’t read, overwhelmed by the lights and sound and decisions. At the register, I realize I forgot my wallet and can’t find the words to explain this to the cashier; can’t do anything other than try and stay conscious. My address, which I can’t remember, is thankfully pre-programmed into the taxi app I can’t identify the icon for. At home, I black out for hours, my body so deeply shutdown I can’t make it to bed, and it is days before I can sit up again without re-triggering an episode.
In her book, The Invisible Kingdom, Meghan O’Rourke describes this level of fatigue as “the body’s cellular conviction that it needed to conserve energy in order to fix whatever was wrong….(a) feeling (that) erased my will, the sense of identity that drives most of us.” The curse is that she called me her Adventure Girlfriend, game for any activity but standing aisle-still. In illness, roles reverse and I become the house-bound, the home-wile, the literally heartbroken, the domesticated horror who wished her domicile would grow legs and roam for her.
In stories, curses happen for a reason: an intergenerational smudge on your family or a moral or ethical failing – rudeness, laziness, hubris, or desire. Even today, some clinicians and researchers unscientifically, incuriously, consider dysautonomia a fear of standing, misinterpreting metrics such as elevated norepinephrine or hypertension as emotionally-triggered, treatable with talk therapy or forced exercise.
Medical professionals faced with me collapsing dramatically ask if I’m scared of needles or doctors, if my mask is cutting off oxygen, if I forgot I took a sleeping pill or overdosed on drugs, if I could just try harder to keep my eyes open. Therapists have proposed grief; my girlfriend suggested panic attacks. At that cardiovascular speed, every mechanism in your body is primed for unspeakable and unpreventable horror and a dysfunctional cardiovascular system can impact neurotransmitters and neuro-cognitive symptoms, a causal loop that lands many people unnecessarily on psychotropic medication dealing with additional cardiac side effects.
To get a cardiology referral, I research the only specialist in town and faint dramatically in front my family medicine clinic’s resident and again in front of the on-call attending, who tells me I “look great today” in the red lipstick and matching dress I wore to prove this wasn’t depression. To get an appointment, I leave monthly voicemails affirming that my symptoms are worsening and impeding tasks of daily living; that the chest pain is sudden, sharp, and nocturnal.
My medical team tries benzodiazepines, which have no impact other than to make me calmer about this catastrophe. They try vasoconstrictors that stimulate the alpha-adrenergic receptors of blood vessels, which leave me hypertensive and hysterical. They try cholinesterase inhibitors and my gastrointestinal system sinks deep into “rest and digest” until I can’t keep food in my body long enough to glean nutritional value. They try calcium channel blockers and beta blockers and leukotriene blockers and histamine blockers and prostaglandin blockers and opioid blockers as though, if we just stopper every malfunctioning mechanism, if we shutdown the bodily machinery overproducing illness, the underlying issues will go away. Everything we try has unintended, catastrophic consequences. At least in Alice in Wonderland the potions are accurately labeled. In another city, my girlfriend’s wife’s tumor shrinks beautifully with the first medication she tries, avoiding radiation all together, and I am grateful at least one field of medicine has its shit together.
Finally, we try a heart failure medication that inhibits the cardiac funny current, the body’s natural pacemaker. Resurrection is a slow cooker, not a defibrillator: the absence of disasters stacking like crossed fingers, the embedded speedometer of too much stretching gum-thin but holding. My once luminous, high voltage syndrome brain flickering on like an unreliable subway map, gesturing the general vicinity. Slowly my runaway heart runs out of batteries.
My posts are not as beautifully written, but I have found some solutions along the way. I hope that you'll have a look. Long COVID: Insights on a journey back to wellness
This is all very relatable. looking forward to the next one!